
Over the past ten years, Santa Catarina has recorded a 30.7% decrease in mortality from HIV/AIDS, which increased from 6.5 to 4.5 deaths per 100 thousand inhabitants. The data noted by medical professionals reveals some nuances in the treatment and diagnosis of the disease in the state.
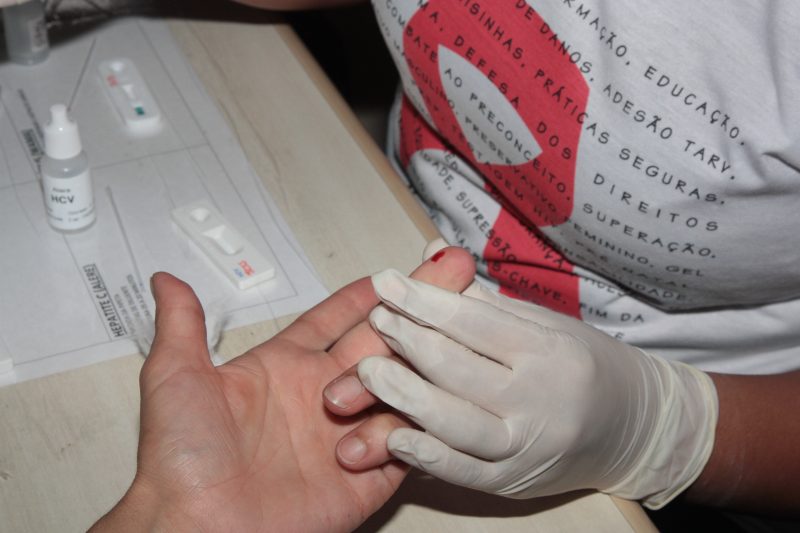 The state reported 455 deaths with HIV or AIDS as the underlying cause, down 7.8% from the 494 deaths reported in 2012. Photo: Divulgação/Prefeitura de Itajaí
The state reported 455 deaths with HIV or AIDS as the underlying cause, down 7.8% from the 494 deaths reported in 2012. Photo: Divulgação/Prefeitura de ItajaíHowever, caution is necessary, infectious disease specialists note. This is because Florianópolis still has a high detection rate and smaller municipalities continue to face challenges.
HIV mortality
According to the epidemiological bulletin released by the Ministry of Health this Monday (11), the state recorded 455 deaths due to HIV or AIDS as the underlying cause in 2022, a 7.8% decrease from the 494 deaths reported in 2012.
However, according to Dr. Alexandre Naime Barbosa, an infectious disease physician, UNESP professor and vice-president of the Brazilian Society of Infectious Diseases, the disease should no longer be a death sentence.
In this regard, Barbosa explained that with proper treatment, it is possible to have an undetectable viral load of the disease and no longer transmit the virus.
“It is important to remember that those on treatment today who have an undetectable viral load have a life expectancy equal to that of the general population and are no longer carriers of HIV,” explains the infectious disease specialist.
Remote locations
Responding to a question about the difficulties in accessing treatment for people living in more remote communities and smaller municipalities in the state, infectious disease physician Regina Walim, manager of the STI/HIV/AIDS and Chronic Infectious Diseases Unit at Dive/SC (Office of Epidemiological Surveillance Santa -Klaus) Katharina) reported that there are plans to fix the problem.
“Today, our focus continues to be basic health care centers where people living with HIV are treated. To ensure patient confidentiality, we have provided training to explain the importance of this secrecy so as not to compromise treatment,” he states.
There are municipalities such as Santiago do Sul, the smallest in the state, located for example in the west of Santa Catarina, with only 1,651 inhabitants. There is only one medical center with 28 employees. Among them are two doctors and two nurses.
According to the infectious disease doctor, all health facilities in Santa Catarina now have PrEP (pre-exposure prophylaxis), in which a person takes medication before being exposed to the HIV virus.
PrEP does not protect against other sexually transmitted infections, so it is often combined with condoms for more complete protection.
Pregnant women
Also, according to the study, the HIV infection rate of pregnant women in the capital of Santa Catarina ranks second in the country: 8.9 (cases per thousand live births).
However, Walim remembers that if this data exists, it is because tests are being done, and the more tests, the more treatments for the disease can be offered.
 The doctor emphasized the importance of monitoring pregnant women with HIV – Photo: TV Brasil/Reproduction/ND
The doctor emphasized the importance of monitoring pregnant women with HIV – Photo: TV Brasil/Reproduction/ND“We want HIV to be diagnosed less and less in the later stages of the disease. Therefore, a pregnant woman needs to be diagnosed either before or preferably in the first months of pregnancy. When I diagnose a pregnant woman and she gives birth, the treatment becomes much more difficult and that is a real challenge,” he says.
Missing Campaigns
Leticia de Assis, who has been an activist and has been living with HIV since 2017, lacks clear campaigns against the disease.
“HIV and AIDS prevention campaigns must be more effective. Young people especially need direct and clear information. This generation has no patience for cut-down information, and at the moment municipal, state and national authorities have not yet found the right tone for dialogue with this population,” he criticizes.
She said many people have never heard of Prep and PEP and have no idea what it’s like to be in a relationship with someone living with HIV and that person can no longer transmit the disease.
Do you know what Prep and Pep are?
PrEP (pre-exposure prophylaxis):
What it is: PrEP involves the regular use of antiretroviral drugs by people who do not have HIV but are at higher risk of contracting the virus.
How it works: Taking these medications regularly helps PrEP block HIV replication in the body, reducing the chance of developing an infection when exposed to the virus.
Use: PrEP is usually prescribed as a tablet to take by mouth daily. There are also alternative protocols, such as on-demand PrEP, depending on the circumstances and medical indications. Indications: Recommended for people in high-risk situations, such as serodiscordant couples, sex workers, people who inject drugs, and other vulnerable populations .
PEP (post-exposure prophylaxis):
What it is: PEP is an HIV prevention strategy aimed at people who have been exposed to the virus, usually through occupational risk situations, needle sticks, or unprotected sex with an HIV-positive or unknown partner.
How it works: Involves using antiretroviral drugs for a short period of time (usually 28 days) after exposure to HIV to prevent infection.
Use: It should be started as soon as possible after exposure, ideally within the first 72 hours, as its effectiveness decreases over time.
Indications: Recommended in situations of recent HIV infection, such as work accidents, sexual assault, or unprotected sex with a high-risk partner.
Information and education about safe sex practices, risk reduction, and informed decision making are important components of combination prevention.
Combination prevention addresses the diversity of situations and behaviors, tailoring prevention strategies to meet the specific needs of different populations and communities. This holistic approach addresses the biological, behavioral and social factors that contribute to the spread of HIV.
Source: Ndmais